Hyperbaric Oxygen Chambers: Is Oxygen Therapy Useful?
What are the benefits and risks of using hyperbaric oxygen chambers? Does this treatment heal diabetic wounds?
Andrew Weil, M.D. | September 12, 2017
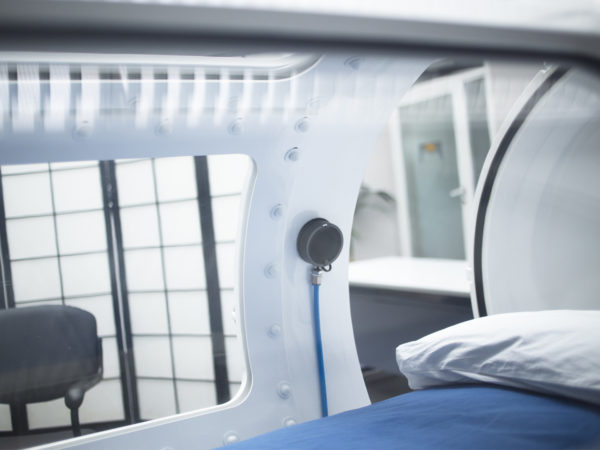
Hyperbaric oxygen therapy (HBOT) involves breathing pure oxygen while in a sealed, pressurized chamber with up to three times normal atmospheric pressure. HBOT is used in conventional medicine for very specific reasons – to treat decompression sickness (“the bends,” a painful and potentially dangerous condition experienced by divers who surface too quickly) and carbon monoxide poisoning, to hasten stroke recovery, and to promote healing of severe skin infections and radiation burns. Medicare has also approved it for treatment of diabetic wounds, although this use remains controversial and is not recommended by the American Diabetes Association.
Tissues in the body require an adequate oxygen supply for normal functioning and even more to survive injury. HBOT increases the amount of oxygen the blood can carry, which raises or temporarily restores normal levels of blood gases and tissue function to promote healing and to fight infection.
In 2002 Medicare approved 30 sessions of HBOT for wounds that haven’t healed after conventional treatment even though then – as now – there is no scientific agreement that the therapy is effective for this purpose. Since then, hundreds of hospitals have installed HBOT facilities at a cost of approximately $500,000. If a patient’s wounds haven’t healed after 30 sessions, hospitals must be able to demonstrate that there has been some improvement in order to be reimbursed for additional treatments. Experts who are dubious about the effectiveness of HBOT treatment for diabetic wounds see the growing use of it as a response to the reimbursement hospitals get from Medicare – $450 for each two-hour session. These sums can add up quickly enough to pay for the investment in the HBOT facilities and generate additional hospital income.
Most HBOT chambers accommodate one person, although larger ones can hold more than a dozen people at a time. During treatment sessions (from 30 minutes to 2 hours) you lie still, try to relax and breathe normally. At the end of the treatment, the chamber is gradually depressurized.
Apart from its medically recommended uses, I’ve seen HBOT promoted as a cure for cancer, a treatment for chronic fatigue syndrome, and a way to reduce allergy symptoms, as well as a beneficial measure for persons with AIDS, arthritis, sports injuries, multiple sclerosis, autism, cerebral palsy, senility, cirrhosis, Lyme disease, and ulcers. I’ve seen no persuasive scientific evidence that HBOT can help patients with these conditions. Nor have I seen evidence that lying in an HBOT chamber provides any general health benefits.
HBOT is not without risk. It can induce claustrophobia, fatigue and headache. More serious potential problems include short-sightedness (myopia) that can last for months after treatment, sinus damage, middle ear rupture and lung damage. HBOT can worsen symptoms of congestive heart failure and can lead to collapsed lung in patients with some types of lung disease. Too much oxygen can also cause seizures. HBOT is not recommended to address any condition in pregnant women except when there are no other treatment options.
Andrew Weil, M.D.
Source:
khn.org/news/hospitals-put-more-stock-in-hyperbaric-therapy-for-diabetics-despite-concerns/