Understanding Measles
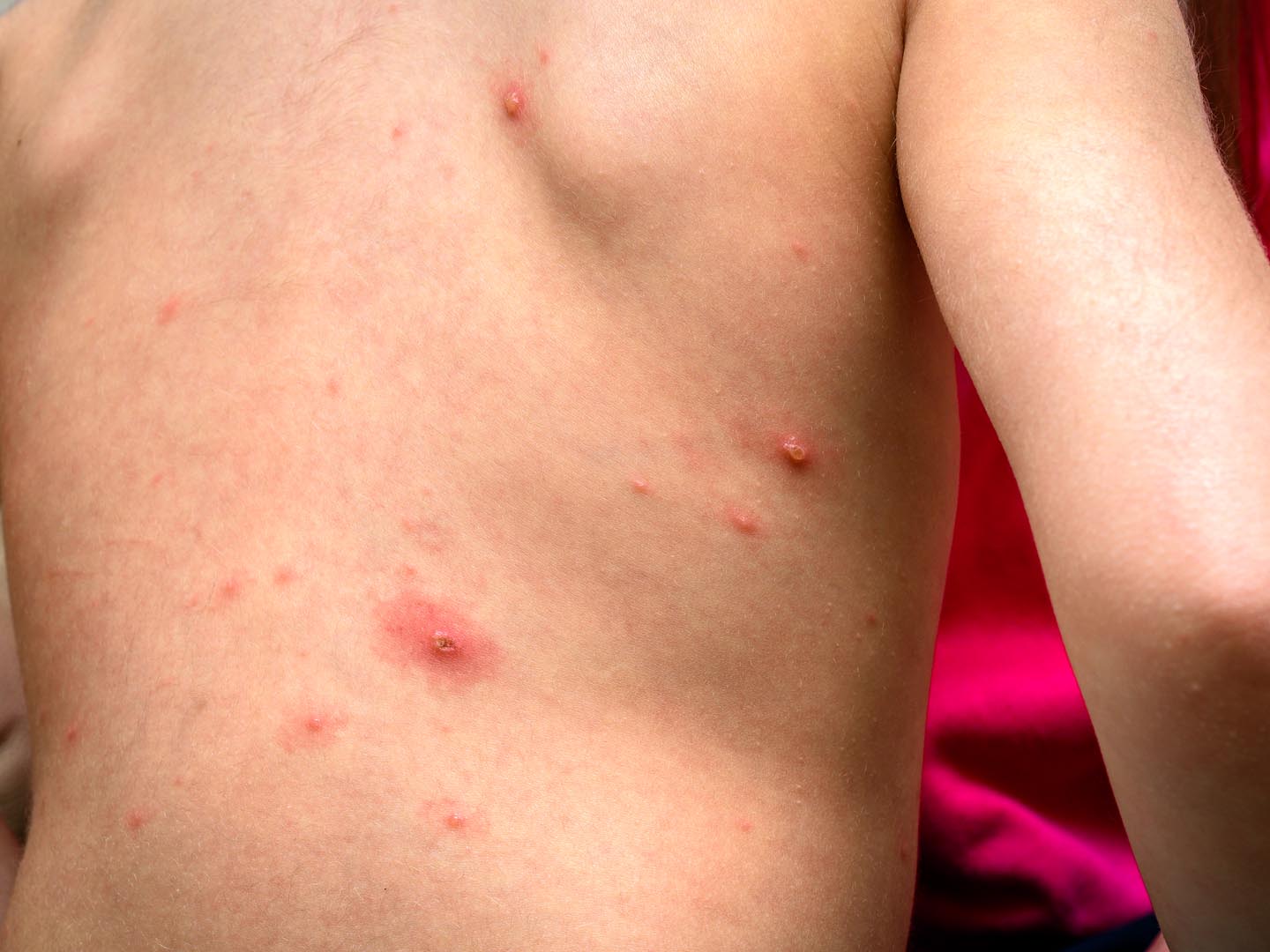
What is measles?
Measles is a highly contagious viral infection that causes a characteristic itchy, red rash and occurs most often in the late winter and spring. Also called rubeola, it is so easily spread that 90 percent of those exposed to the virus will contract measles if they do not already have immunity against it. Approximately 30 million to 40 million cases of measles occur worldwide each year, resulting in close to 1 million deaths.
Fortunately, measles has been kept successfully under control in the United States by the routine administration of MMR vaccination. (“MMR” stands for measles, mumps and rubella; the latter is also sometimes known as German measles.) The vaccine has decreased the incidence of measles by greater than 99 percent. Prior to this vaccine being available, there were approximately 450,000 measles cases and 450 measles-associated deaths in the United States each year. Fewer than 50 cases of measles were reported in the United States in 2004; an extraordinary public-health policy victory. However, vaccination programs are incomplete in much of the world, with global health organizations working hard to address the problem. The widespread, highly infectious nature of the disease and increased public travel to other countries is why vaccination programs are still necessary in the U.S., even though few cases of measles occur.
What are the symptoms of measles?
After exposure, the incubation period runs about 10 to 12 days before symptoms manifest, which usually start with fever, cough, runny nose and conjunctivitis (irritated, red, runny eyes). Body aches and sensitivity to light may also occur. A few days after the first symptoms appear, small red spots with bluish-white centers called Koplik spots may appear on the inside of the cheek. Next, an itchy rash that is blotchy (due to the joining of flat, discolored areas and red, raised patches) appears on the head and face. Typically, the fever increases in severity, often as high as 104-105 F, and the rash continues making its appearance down the body over the next few days. The rash begins to disappear from the head down and other symptoms usually subside after another week.
If one is lucky, the whole course of measles will last only two weeks or less. However, complications can manifest and extend period of illness significantly. About one patient in 10 will get otitis media (an ear infection) and one in 15 will get pneumonia, which can be serious and in some cases, life-threatening. Around one in a thousand contracts encephalitis, which is an inflammation of the brain causing nausea and vomiting, seizures and even coma. Measles can lead to miscarriage and/or low birth-weight babies in pregnant mothers. Young children can also get nausea, vomiting and diarrhea. About one in one thousand cases of measles results in death.
What are the causes?
The measles virus resides in the mucous membranes of the nose, mouth and throat. It is spread through respiratory droplets by coughing and sneezing, where those around the infected person breathe in contaminated droplets from the air. It can also be spread by wiping the nose, then touching an object that might be touched by another person, as in a desk at school or a doorknob. Droplets remain active and contagious on infected surfaces for up to two hours. You contract the virus by putting your fingers in your mouth or nose after touching the infected surface. The infectious period is generally four days prior to and four days after the rash appears.
What is the conventional treatment of measles?
Outside of prevention, there is little one can do for measles but let it run its course. Infants with known exposure to measles can receive the MMR within three days to limit the virulence of the infection. Pregnant or immune-compromised people can receive serum immune globulin injections, which provide pre-formed antibodies to fight the infection. When given within six days of viral exposure, these antibodies can prevent measles or make symptoms less severe.
Antibiotics can be useful if a bacterial complication follows the viral infection, but are essentially useless in treating the virus itself. Tylenol and ibuprofen can help with fever reduction and body aches. Rest and plenty of fluids are recommended as well.
What therapies does Dr. Weil recommend for measles?
Although vaccination with the MMR has all but eradicated the disease in the United States, the recent trend of parents choosing not to vaccinate children could cause the incidence of measles to rise in the U.S. because it is not uncommon to see measles in travelers to this country. This occasionally causes small outbreaks, but could potentially increase in severity as more and more children are not vaccinated. Although the anti-immunizations movement is fueled by parental concerns about the detrimental effects of vaccines, Dr. Weil does not think there is any good evidence linking the vaccines to developmental disorders such as autism and other forms of Pervasive Developmental Disorder (PDD). This is why he made sure that his daughter had all her shots as scheduled. If you’re concerned about side effects, have your pediatrician check your children for any illness prior to vaccination (serious reactions are more likely to occur in sick children). You also may want to look into homeopathic treatments designed to reduce the risk of vaccine reactions.
There is evidence that children with severe measles infections may benefit from vitamin A if they are deficient in it. Vitamin A plays a vital role in immune system health. It also helps the skin and mucous membranes repel bacteria and viruses more effectively.
Measles is more common in less-developed countries, particularly where people suffer from vitamin A deficiency as part of malnutrition. Vitamin A deficiency allows opportunistic infectious diseases such as measles and pneumonia to become deadly. As a general rule, Dr. Weil suggests 15,000 IU of mixed carotenoids daily for adults and 5,000 IU of mixed carotenoids as part of a children’s daily multivitamin, but you should always consult with your pediatrician before beginning supplements.
The measles vaccine is usually given as a combined measles-mumps-rubella (MMR) inoculation, which contains the safest and most effective form of each vaccine. It’s made by taking the measles virus from and adapting it to grow in chick embryo cells in a lab, then modifying the virus to eliminate its virulence. When this modified measles virus is given to a child as part of the MMR vaccine, the virus grows and causes a harmless infection before the immune system gets rid of it. This harmless infection causes 95 percent of children to develop lifetime immunity to the harmful virus found in nature. But a second dose of the vaccine is recommended to protect the 5 percent who didn’t develop immunity after the first dose and to boost immunity in the 95 percent who did.
Doctors recommend that children receive the MMR vaccine between 12 and 15 months of age, and again between 4 and 6 years of age – before entering school. Usually babies are protected from measles for about six months after birth because of the immunity passed on from their mothers. If a child requires protection from measles before 12 months of age – for example, for certain foreign travel or in case of an outbreak – the vaccine can be given as early as 6 months of age. But it needs to be repeated after 12 months of age, when the immune system is more developed and better able to produce the protective antibodies that will provide immunity.
Do you need the MMR vaccine?
You don’t need to be vaccinated if you:
- Had two doses of the MMR vaccine after 12 months of age or one dose of the MMR vaccine plus a second dose of measles vaccine
- Have blood tests that prove you’re immune to measles, mumps and rubella
- Are a man who was born before 1957
- Are a woman who was born before 1957 and you don’t plan to have any more children.
You should be vaccinated if you don’t fit the criteria listed above and you:
- Are a nonpregnant woman of childbearing age
- Attend college, trade school or postsecondary school
- Work in a hospital, medical facility, child care center or school
- Plan to travel overseas or take a cruise.
The vaccine is not recommended for:
- Pregnant women or women who plan to get pregnant within the next four weeks
- People who have had a life-threatening allergic reaction to gelatin or the antibiotic neomycin.
If you have cancer, a blood disorder or another disease that affects your immune system, talk to your doctor before getting an MMR vaccine, and take the normal precautions about close contact with recently vaccinated individuals.
Side effects of the vaccine:
Most people experience no side effects from the vaccine. About 10 percent of people develop a fever between five and 12 days after the vaccination, and about 5 percent of people develop a mild rash. Fewer than one out of a million doses causes a serious allergic reaction.
It was once commonly believed that people who were allergic to eggs couldn’t receive vaccines grown in chick embryos, such as the measles vaccine. But this isn’t true. People with allergies to eggs can safely receive the measles vaccine as well as the combined MMR vaccine.
In recent years, some news reports have raised concerns about a connection between the MMR vaccine and autism. However, extensive reports from the American Academy of Pediatrics, the Institute of Medicine and the Centers for Disease Control and Prevention conclude that there’s no scientifically proven link between the MMR vaccine and autism. In addition, there’s no scientific benefit to separating the vaccines. These organizations note that autism is often identified in toddlers between the ages of 18 months and 30 months, which happens to be about the time children are given their first MMR vaccine. But this coincidence in timing shouldn’t be mistaken for a cause-and-effect relationship.